Definition and Meaning
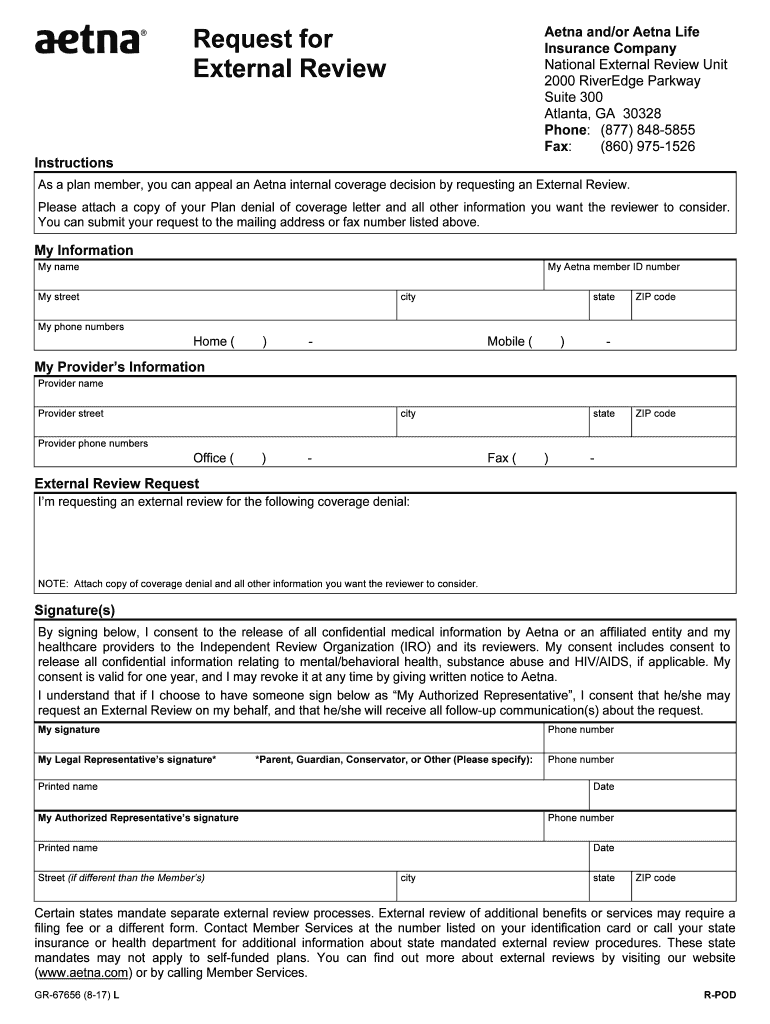
The "Aetna and or Aetna Life" form is a document used by Aetna plan members for specific purposes related to health insurance coverage decisions. This form is typically associated with requests for services like External Reviews of denied coverage claims. Aetna Life Insurance Company is one of the largest healthcare benefits companies in the United States. It offers health insurance products that include medical, dental, and vision plans. Understanding the context and usage of this form is crucial for plan members who need to navigate their coverage options and appeals processes efficiently.
How to Obtain the Aetna and or Aetna Life Form
Members can obtain the "Aetna and or Aetna Life" form via several avenues:
- Online Portal: The most convenient method is through the Aetna member portal, where they can log in and access necessary documents.
- Through Mail: Members can request a physical copy by contacting Aetna's Member Services.
- Customer Support: Direct phone assistance can help guide members on obtaining or filling out the form.
It’s important for members to ensure that they have the most current version of the form for their specific needs.
Steps to Complete the Aetna and or Aetna Life Form
- Personal Information: Start with filling out your personal information, including your Aetna member ID, name, and contact details.
- Provider Information: Input the necessary details about the healthcare provider involved in the decision being reviewed.
- Reason for Submission: Clearly outline the reason for requesting the document, such as a denied coverage decision.
- Consent for Information Release: Sign the consent portion that allows Aetna to access and review medically pertinent information.
- Review and Submit: Double-check each section for accuracy before submitting. Any mistakes could delay the process.
These steps require attention to detail to prevent any delay in processing.
Important Terms Related to Aetna and or Aetna Life
- External Review: A process allowing a third-party to review a denied insurance claim.
- Member ID: Unique identifier for Aetna plan holders, used for verification purposes.
- Consent Form: A document that permits the release of medical information to relevant parties during the review process.
Familiarity with these terms can aid in understanding and completing the form effectively.
Key Elements of the Aetna and or Aetna Life Form
- Member and Provider Details: Essential for identifying the parties involved in the appeal or review.
- Coverage Details: Specific information about the insurance plan and benefits in question.
- Medical Information: May require attaching relevant medical records or past decisions related to the case.
These elements collectively ensure that the form encompasses all required data for processing.
Legal Use of the Aetna and or Aetna Life Form
The form's legal use involves situations where Aetna policyholders need to challenge or question decisions about their insurance coverage. It is important to adhere to legal stipulations to ensure the process is binding and effective:
- Security Compliance: Be mindful of privacy laws like HIPAA when handling medical information.
- Authorization and Compliance: Ensure all provided information is truthful and compliant with Aetna’s guidelines.
Adhering to legal requirements can significantly impact the outcome of the form submission.
State-Specific Rules for the Aetna and or Aetna Life Form
Certain states may have individual processes or additional requirements when using Aetna-related forms. Members are advised to:
- Consult Local Regulations: Understand state-specific guidelines surrounding insurance claims and reviews.
- State Services: Reach out to Aetna's Member Services or a local representative for specific details.
Awareness of these variances is crucial for residents in states with unique rules, as they can directly impact the processing and outcome of the form submission.
Examples of Using the Aetna and or Aetna Life Form
- Denied Treatment Coverage: Requesting an External Review when a medical treatment claim is denied.
- Claim Dispute Resolution: Utilizing the form as part of a process to mediate or contest decisions made by Aetna regarding coverage.
- Appeal for Service Approval: Submitting the form to appeal a prior authorization that was not approved by Aetna.
These scenarios provide a practical look at how the form can be utilized effectively by members seeking to address their insurance coverage issues.