Definition & Meaning
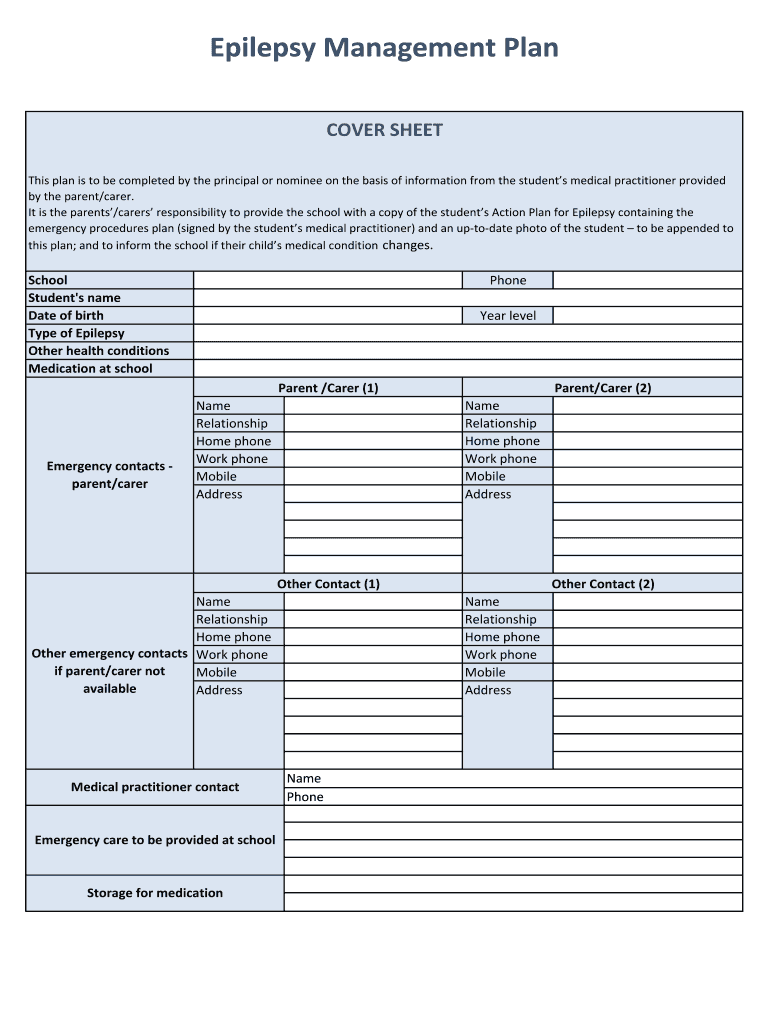
An Epilepsy Management Plan is a comprehensive document crafted to support individuals, particularly students, who experience epilepsy. Its primary objective is to provide detailed guidelines on managing epilepsy in various settings, particularly within schools. The plan encompasses information provided by medical practitioners and parents, thus creating a tailored approach to managing seizures and ensuring safety. It specifies procedures for handling epilepsy-related emergencies, outlining risk minimization strategies across different environments. This plan serves as a critical bridge facilitating communication among parents, schools, and healthcare providers, promoting consistent and effective epilepsy management.
Key Elements of the Epilepsy Management Plan
The Epilepsy Management Plan contains several key components essential for effective epilepsy management:
-
Student Information: Includes the student's name, age, medical history, and specific epilepsy diagnosis.
-
Emergency Contacts: Lists contacts such as parents, guardians, and healthcare providers, ensuring quick communication during emergencies.
-
Seizure Types and Triggers: Detailed descriptions of the student's seizure types and known triggers, aiding in identification and prevention.
-
Medication and Dosage: Lists prescribed medications, dosages, and administration times.
-
Epilepsy Action Plan: Step-by-step procedures to follow during a seizure, ensuring quick and appropriate responses to emergencies.
-
Risk Minimization Strategies: Guidelines for minimizing risks in different environments, such as classrooms or playgrounds.
-
Communication Protocols: Sets out methods for ongoing communication among school staff, parents, and medical professionals.
These elements collectively contribute to a comprehensive, individualized strategy for managing epilepsy within the school environment.
How to Use the Epilepsy Management Plan
The plan is utilized by various stakeholders who play roles in supporting the student. To effectively use the Epilepsy Management Plan:
-
Parents and Guardians: Should ensure that the plan is accurate and up-to-date, reviewing it regularly with healthcare providers and school staff.
-
School Staff: Must familiarize themselves with the plan, understand steps for seizure management, and recognize the student's specific needs and triggers.
-
Medical Personnel: Provide expert input on medical management and emergency care procedures, ensuring the plan reflects best practices in epilepsy care.
Consistency in using the plan allows stakeholders to provide coordinated care, reducing the impact of epilepsy on the student's learning and social experiences.
Steps to Complete the Epilepsy Management Plan
Effective completion of the Epilepsy Management Plan involves several important steps:
-
Gather Medical Information: Collaborate with healthcare providers to gather necessary medical insights and epilepsy-specific information.
-
Engage with Parents: Collect detailed input from parents or guardians about the student's seizure history and emotional and behavioral insights.
-
Consult School Personnel: Include information from teachers and school health staff about environmental factors and necessary accommodations.
-
Draft the Plan: Use the information gathered to draft a comprehensive plan. Ensure all sections are filled accurately and thoroughly.
-
Review and Approve: Hold review meetings with all involved stakeholders to finalize the plan, making adjustments as necessary.
-
Implementation and Training: Implement the plan and train school staff on procedures and guidelines to ensure preparedness.
-
Regular Review and Update: Schedule regular reviews to update the plan and incorporate any changes in the student's condition or school circumstances.
These steps help build a robust document that can effectively guide all parties involved in school-time epilepsy management.
Why You Need an Epilepsy Management Plan
Having an Epilepsy Management Plan is crucial for several reasons:
-
Safety: It ensures the student's safety by preparing caregivers and educators to respond swiftly and effectively to seizures.
-
Consistency: Provides a consistent approach across different caregivers and environments, reducing variability in care.
-
Collaboration: Encourages collaboration among families, schools, and medical providers, enhancing communication and understanding.
-
Documentation: Serves as a legal document outlining the agreed action plan, protecting both the student and the caregivers by documenting consented approaches to management and care.
This plan is not only an essential safety net but a tool that empowers all involved to provide the best possible care and support.
Who Typically Uses the Epilepsy Management Plan
The Epilepsy Management Plan is typically used by:
-
Parents/Guardians: As primary caregivers, they ensure that health concerns are communicated effectively and accurately to the school.
-
School Staff and Educators: Teachers, school nurses, and administrators use the plan to support and manage students with epilepsy during school hours.
-
Healthcare Providers: Physicians and epilepsy specialists use their medical expertise to inform the plan and recommend best practices.
-
Emergency Responders: The plan is essential for any on-scene medical response professionals who may be called to a school during a seizure event.
This collaborative approach enables integrated care strategies, contributing to improved quality of life and educational outcomes for students with epilepsy.


Important Terms Related to Epilepsy Management Plan
Understanding key terms associated with the Epilepsy Management Plan can enhance its effective implementation:
-
Seizure: A sudden surge of electrical activity in the brain that affects how a person feels or acts.
-
Triggers: Factors or stimuli like stress or flickering lights that can potentially provoke seizures.
-
Aura: A sensation or set of symptoms experienced at the onset of certain seizures, serving as a warning signal.
-
Postictal State: The altered state of consciousness after an epileptic seizure, typically involving confusion or tiredness.
-
Antiepileptic Drugs (AEDs): Medications prescribed to control seizures. Understanding AEDs' dosages and side effects is crucial for management planning.
These terms represent foundational concepts that aid in developing a comprehensive understanding of the plan's objectives and procedures.
Legal Use of the Epilepsy Management Plan
From a legal perspective, the Epilepsy Management Plan is a critical document. In the U.S., it aligns with laws such as the Individuals with Disabilities Education Act (IDEA) and Section 504 of the Rehabilitation Act, which mandate appropriate accommodations in educational settings for students with disabilities.
-
IDEA Compliance: Ensures that students receive an Individualized Education Plan (IEP) reflecting their specific epilepsy management needs.
-
Section 504 Requirements: Covers the development of a 504 Plan if needed, preventing discrimination based on a medical condition and ensuring reasonable accommodations.
Legal adherence ensures that students' educational rights are protected while also obligating schools to provide necessary supports and accommodations.