Definition & Meaning
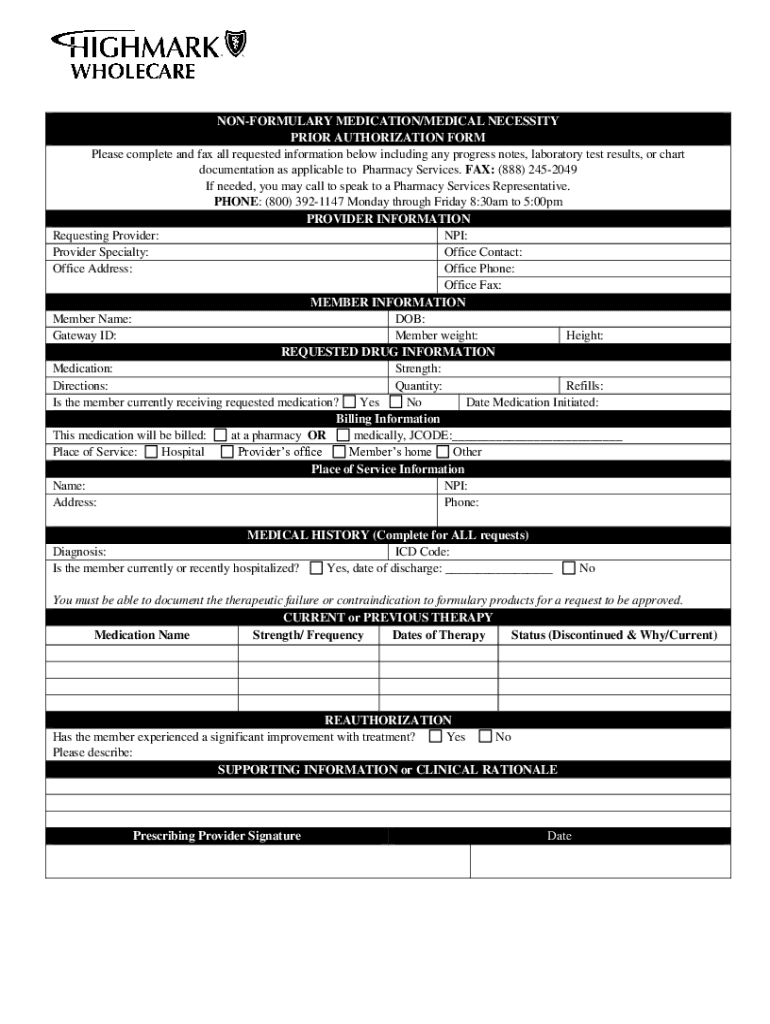
Prior Authorization Criteria for Non-Formulary Medications refer to the guidelines that healthcare providers and patients must adhere to when requesting coverage for medications that are not listed in a health plan's formulary. A formulary is a list of prescription medications that are approved for coverage by a health insurance policy or plan. Non-formulary medications typically require prior authorization because they are usually more expensive or are considered less cost-effective than formulary options. The aim of establishing criteria for these authorizations is to ensure that such medications are prescribed appropriately and to manage healthcare costs while maintaining high-quality care.
Key Elements of the Prior Authorization Criteria Non-Formulary Medications
- Clinical Justification: The need for the medication must be clinically justified. This may include explanations for why formulary medications are not suitable for the patient, such as documented adverse reactions or contraindications.
- Patient History: Detailed patient history may be required, encompassing past treatments, responses to previous medications, and current health conditions. This helps in evaluating the necessity of the non-formulary drug.
- Physician's Statement: A statement from the prescribing physician is often necessary. This document outlines the rationale for prescribing the non-formulary medication and provides supporting evidence from medical records.
Steps to Complete the Prior Authorization Criteria Non-Formulary Medications
- Initiation by Healthcare Provider: The process is typically initiated by the healthcare provider who prescribes the medication. They must fill out the required forms and submit any relevant documentation.
- Gathering Required Information: Providers need to compile comprehensive information, including patient records and the reason for selecting a non-formulary medication.
- Submission: Once the form and documentation are complete, they must be submitted to the insurance company for review. Submission methods can vary, sometimes requiring fax or online submission via a dedicated portal.
How to Use the Prior Authorization Criteria Non-Formulary Medications
Healthcare providers use the prior authorization criteria to evaluate whether a non-formulary medication is necessary for their patient's treatment plan. Providers must ensure all criteria are met and accurately documented before submission to improve the chances of authorization approval. Patients should coordinate with their healthcare provider to ensure all necessary steps are taking place for a timely response from insurers.
Process Overview
- Provider Assessment: Continuous assessment by the healthcare provider to determine if the patient’s condition warrants the use of non-formulary medications.
- Documentation: Accumulate necessary paperwork that supports the use of the desired non-formulary medication.
- Authorization Request: Submit an officially completed request form along with all required documents to the patient's insurance provider.
Who Typically Uses the Prior Authorization Criteria Non-Formulary Medications
These criteria are primarily used by healthcare providers and other medical professionals who prescribe medications. Patients and their families are also actively involved in the process since they need to be aware of the steps required to obtain coverage for non-formulary medications. Insurance companies use these criteria to decide whether to approve or deny requests based on medical necessity and cost-effectiveness.


Eligibility Criteria
Eligibility for non-formulary medication coverage often requires:
- Proven Need: The patient must demonstrate a medical need for the non-formulary medication that can’t be substituted with a formulary option.
- Lack of Alternatives: All possible formulary alternatives must have been tried and proven ineffective or unsuitable for the patient.
- Compliance: Providers must comply with insurance directives, including correct filling and timely submission of required forms.

Legal Use of the Prior Authorization Criteria Non-Formulary Medications
The use of these criteria is governed by healthcare laws and insurance regulations which dictate the appropriate documentation and procedures required to ensure authorization. These legal frameworks are designed to protect patients, ensure fair processes, and manage healthcare spending efficiently. Compliance with regulations like the Health Insurance Portability and Accountability Act (HIPAA) is crucial to maintain the confidentiality and security of patient information throughout the process.
Important Terms Related to Prior Authorization Criteria Non-Formulary Medications
- Formulary: A list of medications approved for coverage by a health insurance plan.
- Prior Authorization: The process of obtaining approval from an insurance provider before a prescription is filled.
- Non-Formulary Medication: A drug not included in an insurance plan's formulary, often requiring special approval for use.
- Clinical Necessity: Justification based on clinical evidence that a certain medication is needed to effectively treat a patient's condition.
- Prescribing Provider: The healthcare professional responsible for providing documentation and justification for the use of non-formulary medications.