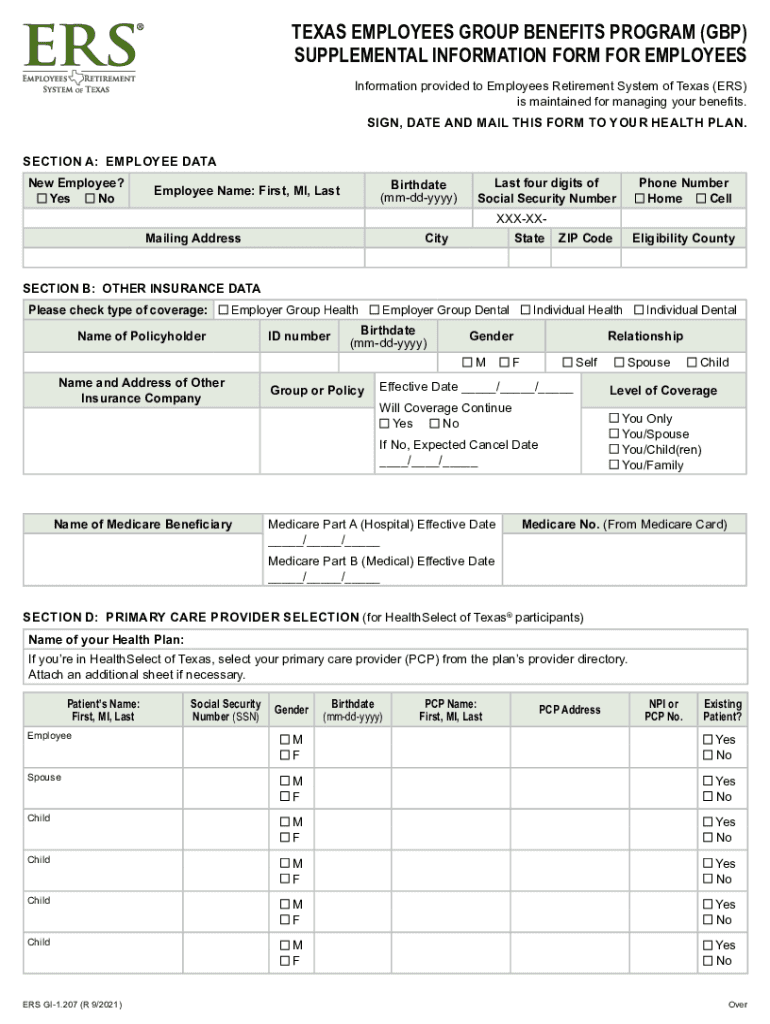
Definition and Purpose of the Texas Employees Group Benefits Program (GBP) Supplemental
The Texas Employees Group Benefits Program Supplemental is a crucial document for employees participating in this state-managed benefits program. The purpose of the supplemental form is to gather additional information that supports the administration and processing of benefits entitlements. It plays an integral role in ensuring that all necessary data, such as insurance coverage details and dependent information, is accurately captured to facilitate the issuance of a health care identification card upon successful enrollment.
Core Components and Information Required
Key components collected through the form include:
-
Employee Personal Information: Details like name, address, and employee identification number are essential to establish a connection with the primary benefits program.
-
Insurance Details: Information about any existing health insurance plans is gathered to coordinate benefits and avoid duplication of coverage.
-
Medicare Information: Employees enrolled in Medicare must provide their Medicare Policy number to streamline processing and ensure benefits compatibility.
-
Dependent Information: This section records data about dependents, particularly those not living in the household, affecting the calculation and allocation of benefits.
How to Obtain the Texas Employees Group Benefits Program Supplemental
Securing the GBP Supplemental form is accessible through a few methods designed for ease and convenience:
-
Online Download: Most participants can download the form directly from the official government or benefits program website.
-
HR Departments: The form may also be available via the human resources departments of participating employers.
-
Mail or In-Person Requests: For those who require physical copies, requesting a mailed version or picking one up from relevant offices is possible.
Steps to Complete the Texas Employees Group Benefits Program Supplemental
Completing the GBP Supplemental involves several steps to ensure accuracy and completeness:
-
Collect Necessary Documents: Gather personal identification, insurance policies, and Medicare cards if applicable.
-
Fill Out Personal Information: Include full name, address, and employee identification details accurately.
-
Input Insurance Information: Clearly mention existing health insurance plans to enable effective coordination.
-
Detail Medicare Policy: For Medicare participants, provide policy numbers accurately to avoid processing delays.
-
Provide Dependent Information: Carefully complete this section to reflect accurate details on dependents impacting the health card issuance.
Who Typically Uses the Texas Employees Group Benefits Program Supplemental
The GBP Supplemental form caters primarily to:
-
State Employees: Eligible employees working for state agencies or public institutes.
-
Dependents of State Employees: Spouses or children requiring inclusion in the benefits program.
-
Retirees: Former state employees maintaining certain benefits post-retirement.


Key Elements of the Texas Employees Group Benefits Program Supplemental
Critical elements within the GBP Supplemental form are:
-
Insurance Coordination: Essential to coordinating between state benefits and any other insurance.
-
Eligibility Verification: Ensures applicants meet program eligibility criteria.
-
Data Accuracy: Vital for accurate processing leading to smooth benefits provision.
Required Documents for the Texas Employees Group Benefits Program Supplemental
Completion of the GBP Supplemental demands supporting documents to verify and cross-check provided information:
-
Identification Documents: Such as a driver's license or state ID.
-
Insurance Policies: Details of other health insurance plans.
-
Medicare Cards: For those covered under Medicare.
Legal Use of the Texas Employees Group Benefits Program Supplemental
The GBP Supplemental form carries significant legal implications to ensure compliance and transparency:
-
Data Protection: All information must be used in accordance with data protection regulations.
-
Legal Accuracy: Providing false information can lead to penalties or loss of benefits eligibility.
Disclosure Requirements
Legal use mandates full disclosure of any relevant insurance coverage or changes in personal or dependent status impacting benefits entitlement.