Definition & Meaning
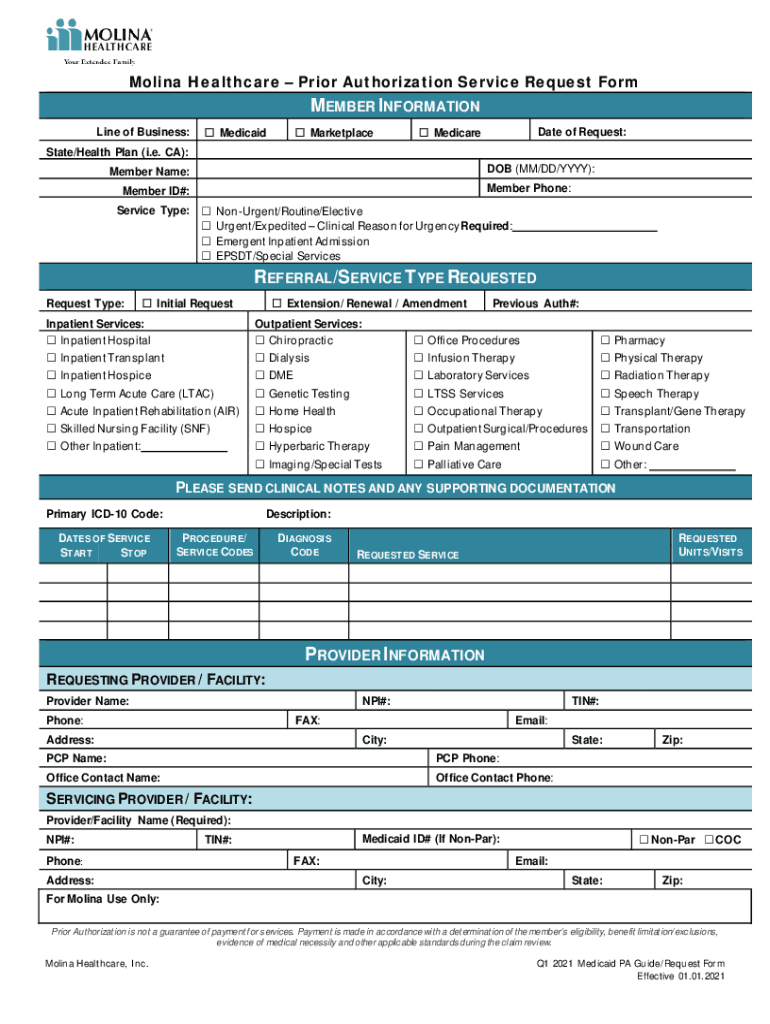
The Molina Healthcare - Prior Authorization Service Request Form is a critical document used to request approval for specific medical services under Molina Healthcare's Medicaid, Marketplace, and Medicare lines. It is an essential tool for healthcare providers to ensure that medical services are authorized prior to being rendered, which aids in aligning with the insurance provider's protocols and coverage policies.
Key Features
- Medical Service Approval: The form is primarily used to secure pre-approval from Molina Healthcare for medical procedures or treatments under its coverage plans.
- Coverage Clarity: It helps clarify the services that will be covered under a patient's specific insurance plan, preventing unexpected expenses and coverage denials.
Additional Considerations
- No Guarantee of Payment: It's important to note that obtaining prior authorization does not automatically guarantee payment. Other conditions like medical necessity and eligibility requirements are taken into account during the claim review process.
How to Use the Molina Healthcare - Prior Authorization Service Request Form
Using the Molina Healthcare - Prior Authorization Service Request Form effectively involves a series of steps to ensure compliance and accuracy.
Step-by-Step Instructions
- Gather Necessary Information: Collect all relevant patient details, including member ID, diagnosis, and provider information.
- Service Details: Clearly outline the type of service being requested, including CPT codes if applicable.
- Attach Clinical Documentation: Provide supporting clinical documentation that justifies the medical necessity of the requested service.
- Review and Double-check: Ensure all fields are completed accurately to avoid delays in processing.
- Submit the Form: Use the specified submission methods, such as via fax or an online portal, to send the form for review.
Steps to Complete the Molina Healthcare - Prior Authorization Service Request Form
Completing this form requires attention to detail and adherence to specific guidelines.
Detailed Completion Guide
- Patient Information: Start by entering all patient-specific details, ensuring accuracy with names, dates, and identification numbers.
- Service Type: Specify the service type requested, making sure to include any specific codes or descriptions that are applicable.
- Provider Information: Accurately fill out details for the provider delivering the services, along with contact information.
- Clinical Details: Attach detailed clinical documentation to substantiate the service request.
Why Should You Use the Molina Healthcare - Prior Authorization Service Request Form
The use of this form provides significant advantages in managing healthcare service requests.
Benefits
- Prevents Financial Surprises: Ensures services are pre-approved, reducing the risk of unexpected denial of coverage.
- Streamlines Communication: Facilitates clear communication between healthcare providers and insurers concerning service coverage.
- Enhances Efficiency: Streamlines the administrative process associated with healthcare service requests.
Who Typically Uses the Molina Healthcare - Prior Authorization Service Request Form
This form is primarily used by healthcare providers who are part of Molina Healthcare's network or are seeking approval for covered services for their patients.


Key Users
- Healthcare Providers: Doctors and medical staff utilize it to request authorization for treatments.
- Administrative Personnel: Hospital or clinic administrators manage the submission and tracking of the form.
Important Terms Related to Molina Healthcare - Prior Authorization Service Request Form
Understanding specific terms within the authorization process can enhance comprehension and effective usage.
Glossary of Terms
- Prior Authorization: A pre-approval process for certain medical services to ensure coverage and necessity.
- CPT Code: Current Procedural Terminology code used to describe the medical service rendered.
- Medical Necessity: A justification for the service based on clinical need and patient benefit.
Key Elements of the Molina Healthcare - Prior Authorization Service Request Form
There are several crucial elements that need to be accurately filled out within the form.
Critical Sections
- Member Information: Includes patient demographics and insurance details.
- Requested Service Description: Detailed information about the medical service or procedure requested.
- Provider Details: Information about the healthcare provider requesting the service, including NPI and tax ID.
Form Submission Methods
There are various methods available for submitting the Molina Healthcare - Prior Authorization Service Request Form.
Available Submission Options
- Online Submission: Through an online portal provided by Molina Healthcare.
- Fax Submission: The form can be faxed to the appropriate department for processing.
- Mail Submission: For those preferring traditional mail, forms can be sent to a designated mailing address as per Molina Healthcare guidelines.
Required Documents
Certain documentation must accompany the Molina Healthcare - Prior Authorization Service Request Form to facilitate processing.
Accompanying Documentation
- Clinical Records: Relevant medical records supporting the service request.
- Patient History: A detailed history that underscores the necessity of the requested service.
- Authorization Code: Any pre-existing authorization codes relevant to the patient's plan.
Who Issues the Form
Understanding the issuer provides context about the form’s authority and purpose.
Issuing Body
- Molina Healthcare: This organization issues the Prior Authorization Service Request Form and handles its processing to manage service authorizations for patients under its care.
Eligibility Criteria
Determining who qualifies to use this form is vital for appropriate utilization.

Criteria for Use
- Plan Coverage: The patient must be enrolled in a Molina Healthcare plan.
- Service Requirement: The requested service must require prior authorization according to the specific plan rules.
Legal Use of the Molina Healthcare - Prior Authorization Service Request Form
The legal implications of using the form ensure compliance with healthcare regulations.
Compliance Considerations
- HIPAA Regulations: Personal health information must be handled according to HIPAA standards.
- Authorization Requirements: Completing the form as required by legal standards and insurance policy guidelines ensures legally sound processes.
Versions or Alternatives to the Molina Healthcare - Prior Authorization Service Request Form
Understanding if there are different versions or related forms can assist in selecting the correct document.
Form Alternatives
- State-Specific Variations: Some states might have adapted forms to meet local regulatory requirements.
- Plan-Specific Forms: Certain plans may offer alternative documentation depending on service complexity or type.
By detailing the Molina Healthcare - Prior Authorization Service Request Form in these various dimensions, this content aims to provide healthcare providers and administrative professionals with a comprehensive understanding of the form's use, purpose, and submission process.