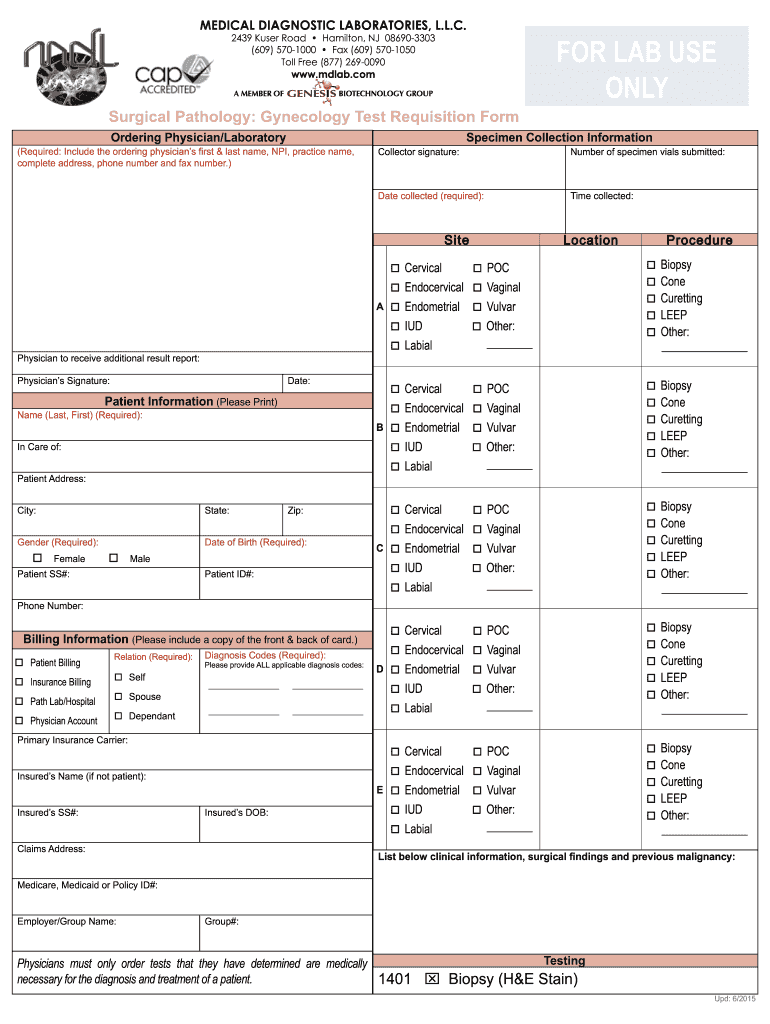
Definition and Meaning of the Anatomic (Surgical) Pathology Test Requisition Form
The Anatomic (Surgical) Pathology Test Requisition Form is a vital document used in the medical field to officially request pathology tests. This form is predominantly utilized by healthcare providers to order procedures that diagnose diseases by examining tissue samples obtained during surgeries or biopsies.
Key terms and definitions related to this form include:
- Pathology: The medical specialty that focuses on the diagnosis of disease through the examination of organs, tissues, and bodily fluids.
- Surgical Pathology: A branch of pathology that deals specifically with specimens obtained during surgical procedures.
- Requisition Form: A document that makes a formal request for medical tests or procedures to be conducted.
Understanding the purpose of this form is essential in ensuring proper documentation and processing of medical tests, which are critical for patient care and treatment planning.
Steps to Complete the Anatomic (Surgical) Pathology Test Requisition Form
Filling out the Anatomic (Surgical) Pathology Test Requisition Form accurately is crucial for effective communication within the medical team and for the efficient handling of test orders. Here are detailed steps to guide users through the process:
-
Patient Information:
- Full name, date of birth, and contact details.
- Insurance information may also be required to facilitate billing.
-
Physician Information:
- Complete details of the healthcare provider requesting the test, including name, contact number, and medical license number.
-
Specimen Details:
- Include specific information about the type of specimen being submitted (e.g., biopsy, tissue).
- Document collection methods or procedures taken when obtaining the sample.
-
Test Selection:
- Indicate the specific pathology tests being requested, ensuring that only medically necessary tests are ordered.
- Different tests may require different codes or descriptions; check for accuracy.
-
Billing Information:
- Include necessary details for billing purposes, especially if the patient has insurance.
-
Diagnosis Codes:
- Attach appropriate ICD codes related to the patient's diagnosis, as this aids in justifying the medical necessity for the tests ordered.
-
Signature:
- The physician's signature is often required to authenticate the order.
-
Submission Instructions:
- Follow the designated instructions for submitting the form, whether electronically, by mail, or in person.
Completing the form carefully helps ensure that the pathology testing occurs smoothly, contributing vital information for evaluating the patient's health condition.
Key Elements of the Anatomic (Surgical) Pathology Test Requisition Form
The Anatomic (Surgical) Pathology Test Requisition Form comprises several key elements that ensure comprehensive and accurate submissions. Each element plays a distinct role in the overall process of pathology testing and diagnosis. Important components include:
-
Patient Identification:
- Essential for linking test results with the correct individual.
-
Ordering Physician Information:
- Provides context on who is requesting the test, ensuring accountability.
-
Specimen Type and Collection Method:
- Indicates the nature and handling of the sample, which can impact test results.
-
Requested Tests:
- Clearly states which tests are necessary for diagnostic purposes, ensuring clinical relevance.
-
Billing and Insurance Details:
- Facilitates smoother processing for insurance claims, speeding up the payment for services rendered.
-
Diagnosis Codes:
- Helps to establish the medical necessity for the requested tests, crucial for proper insurance processing.
By ensuring all these elements are included accurately, healthcare providers bolster the effectiveness of the pathology process, improving patient outcomes.
Who Typically Uses the Anatomic (Surgical) Pathology Test Requisition Form
Several professionals in the healthcare field typically utilize the Anatomic (Surgical) Pathology Test Requisition Form. Understanding the typical users helps clarify the interconnectedness of roles within the medical profession regarding pathology testing:
-
Pathologists: They are the end-users of the form, interpreting the results of the tests ordered.
-
Surgeons: Often the individuals requesting the pathology tests based on surgical findings.
-
Oncologists: Frequently require pathology tests to ascertain the nature of tumors and develop treatment plans.
-
General Practitioners: Sometimes order pathology tests for their patients and rely on the accurate completion of the requisition.
-
Medical Assistants or Administrative Staff: These individuals often help in filling out or managing the forms on behalf of the healthcare providers, ensuring all details are complete before submission.
Understanding the typical users ensures that the requisition process is streamlined and that each party involved knows their responsibilities.


Important Terms Related to the Anatomic (Surgical) Pathology Test Requisition Form
Familiarity with the terminology related to the Anatomic (Surgical) Pathology Test Requisition Form establishes a solid foundation for effective communication and form utilization within the medical environment. Key terms include:
- Biopsy: The removal of tissue for examination, often ordered based on initial findings during a medical examination.
- ICD Codes: The International Classification of Diseases codes that classify diseases for billing and research, indicating the medical necessity of tests.
- Specimen: Any material collected for medical examination, such as tissue samples.
- Pathology Report: The document generated post-testing that includes findings from the pathology tests.
Understanding and accurately using these terms fosters clearer communication between healthcare providers, enhances procedural understanding, and ensures adherence to professional standards.