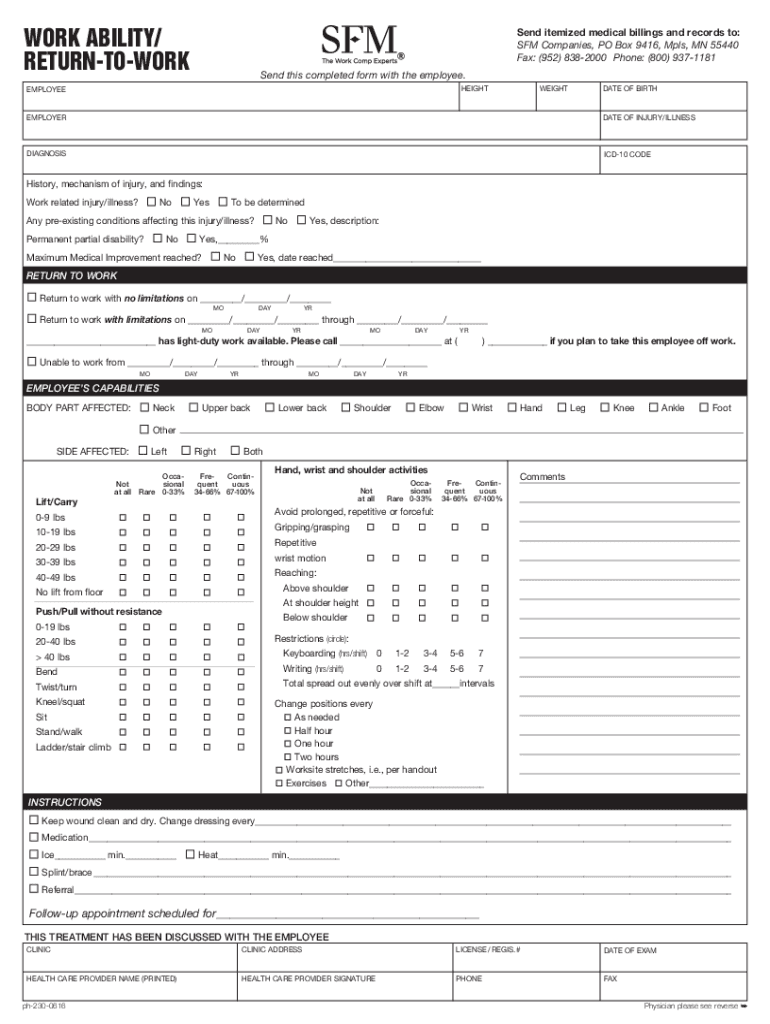
Definition and Purpose of the Work Ability and Return-to-Work Form
The "Work Ability and Return-to-Work Form" serves as a critical document completed by a treating physician to assess an injured employee's capacity to resume work duties. This form facilitates streamlined communication between healthcare providers and employers, ensuring that any limitations or recommendations regarding an employee's return to work are clearly documented. Typically, this form includes sections related to medical evaluations, potential work restrictions, and suggestions for job modifications, which are vital for a facilitated reintegration into the workplace.
How to Use the Work Ability and Return-to-Work Form
- Obtain the Form: Usually accessible through an employer's human resources department or directly from the physician's office handling the treatment.
- Complete the Form: The treating physician will fill out the form, detailing the employee's medical status, work capabilities, and any restrictions.
- Review and Discuss: The completed form should be reviewed by both the employee and employer to align on the work accommodation plans.
- Submit to the Employer: Once all parties are in agreement, the form is submitted to the employer to be placed in the employee’s medical file.
Steps to Complete the Form
- Section for Employee Information: Include the employee's full name, job title, and contact details.
- Injury Details: Document the type and extent of injury, and the date it occurred.
- Medical Assessment: The physician details current medical conditions, treatments received, and progress.
- Work Restrictions: Note any limitations affecting job duties, such as weight lifting restrictions or need for frequent breaks.
- Recommended Modifications: Provide suggestions for adapting the work environment or duties to ensure safety and productivity.
- Signatures and Date: Both the physician and the employee must sign the form, verifying the information and acknowledging the plan.
Who Typically Uses the Form
- Employees: To communicate medical status and work capability.
- Employers: To assess and accommodate workplace adjustments.
- Healthcare Providers: To give professional evaluations and recommendations.
- Insurers: Sometimes used to evaluate claims and determine coverage of work-related injuries.


Legal Considerations
The form must comply with federal and state occupational health and safety standards. It is also aligned with privacy laws that protect the employee's medical information. Legal compliance ensures both employers and employees meet legislative requirements, thus avoiding potential disputes or fines.
Key Elements of the Form
- Physician’s Evaluation: Crucial for understanding the employee's capacity for work.
- Work Restrictions: Clearly states what the employee can and cannot do.
- Return-to-Work Date: Provides guidance on when the employee is likely able to resume duties.
- Signatures: Essential for form validity, demonstrating agreement by involved parties.
State-Specific Rules and Differences
Regulations governing the use of the "Work Ability and Return-to-Work Form" may vary by state. Employers should consult local labor offices to ensure compliance with state-specific laws concerning employee health records and return-to-work protocols. Some states might have additional forms or documentation requirements.
Digital vs. Paper Versions
While traditionally available as a paper document, digital versions of the form can streamline processing and sharing among stakeholders. Platforms like DocHub allow for electronic completion and signing, which enhances convenience and efficiency, providing options for securing the document with encryption and passwords.
Relevant Examples
Consider an employee who sustained a back injury while lifting heavy equipment. The form might outline specific recommendations, such as limiting lifting to no more than 10 pounds. Alternatively, an employee recovering from carpal tunnel surgery might have a form indicating a need for flexibility in typing requirements or job rotation to prevent re-injury.
Importance of the Form
Using this form is crucial in managing workplace injuries effectively. It supports the injured employee's recovery by ensuring appropriate adjustments and facilitates smooth transitions back to the workplace, thereby minimizing disruptions and maintaining productivity. Employers benefit by ensuring compliance with occupational health regulations, reducing potential liability.
Providing a comprehensive and in-depth understanding of the "Work Ability and Return-to-Work Form" ensures that all parties involved appreciate its role and can utilize it effectively in the rehabilitation and reintegration of injured employees.