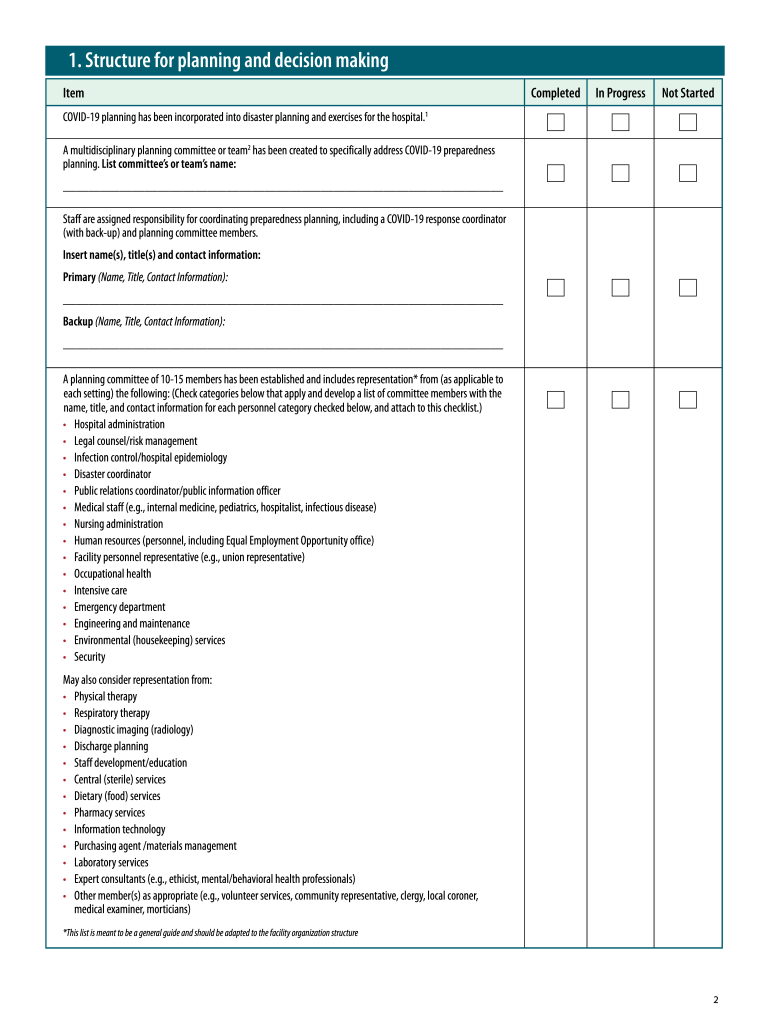
Definition and Meaning
In the context of "Guidance for health system contingency planning during," this term refers to the comprehensive set of instructions or recommendations developed to aid health systems in preparing for and responding to unexpected events, such as pandemics or natural disasters. This guidance ensures that hospitals and related health institutions can maintain essential services during crises. It usually includes plans for operational continuity, resource allocation, patient care, and communication strategies.
Key Components of Health System Contingency Planning
- Emergency Preparedness Plans: Tailored strategies to respond to various emergencies, ensuring continuity of services.
- Resource Management: Guidelines for effectively managing medical supplies, staff, and facilities.
- Communication Protocols: Structured communication strategies aimed at maintaining clarity and coordination internally and with external partners.
- Training and Simulation Exercises: Regular training for staff to handle emergency scenarios effectively and confidently.
How to Use the Guidance for Health System Contingency Planning During
Health systems should incorporate the guidance into their existing emergency preparedness frameworks. The document should be used as a roadmap to align current practices with recommended protocols for improved resilience during crises.
Implementation Steps
- Assess Current Preparedness Levels: Review existing plans to identify gaps.
- Integrate Recommendations: Update procedures and protocols as necessary.
- Train Staff: Implement training sessions to ensure all personnel understand and can effectively execute the plan.
- Conduct Drills: Regularly perform drills to test various components of the contingency plans.
Practical Examples
- Hospitals may develop a tiered response system outlined in the guidance to navigate varying threat levels, such as flu seasons versus pandemic situations.
- Adjusting staffing models to support an increase in patient numbers during a crisis.
Steps to Complete the Guidance for Health System Contingency Planning During
Completing this guidance involves several methodical steps aimed at building a robust plan that addresses the unique needs of a health system.
Detailed Steps
- Initial Review: Gather all stakeholders to review the existing health system capabilities.
- Customize the Guidance: Adapt the guidelines to suit the specific needs and resources of your institution.
- Allocate Resources: Identify and allocate necessary resources, including funding, staff, and equipment.
- Develop Protocols: Draft detailed procedures for various emergency scenarios.
- Create a Communication Plan: Ensure clear communication channels and protocols are established.
- Evaluate and Revise: Regularly evaluate the effectiveness of the guidance and update it as needed.
Examples of Completed Tasks
- Development of a partnership with local governmental bodies for resource sharing in emergencies.
- Establishing a centralized communication hub within the hospital to coordinate during high-stress situations.
Key Elements of the Guidance for Health System Contingency Planning During
Understanding and effectively implementing this guidance requires focus on several critical elements, which collectively ensure comprehensive preparedness.
Core Elements
- Risk Assessment: Identifying potential threats and their impacts on health systems.
- Resource Allocation: Strategic distribution of resources to ensure readiness.
- Training Programs: Preparing staff through simulation exercises and continued education.
- Operational Continuity: Maintaining essential services without interruption.
Examples in Practice
- Creating a resource stockpile specific to anticipated disasters, ensuring availability during times of high demand.
- Implementing a flexible staffing model that can quickly adapt to changing needs.
State-specific Rules for the Guidance for Health System Contingency Planning During
Different states may have unique regulations and requirements concerning health system contingency plans. It's essential to align local practices with statewide mandates.
Notable State Differences
- Regulatory Standards: Some states have stricter regulatory standards for emergency preparedness.
- Funding Models: Availability of state funding for emergency preparedness can vary.
- Reporting Requirements: States might have specific metrics that need regular reporting.
Real-World Examples
- In California, hospitals might need to comply with seismic readiness standards as part of their contingency planning.
- States in hurricane-prone areas may have additional protocols related to severe weather preparedness.
Legal Use of the Guidance for Health System Contingency Planning During
Implementing the guidance can have legal implications, especially concerning patient care and the standard of care expectations during emergencies.
Legal Framework
- Compliance with Federal and State Laws: Ensuring health systems meet legal obligations during crisis situations.
- Liability Concerns: Understanding the risks and potential liabilities involved in emergency response.
- Documentation: Keeping thorough records of preparedness activities for accountability.
Examples of Legal Considerations
- Ensuring compliance with HIPAA regulations during the deployment of digital communication systems in emergencies.
- Verification that emergency protocols meet occupational safety standards to protect staff.
Who Typically Uses the Guidance for Health System Contingency Planning During
This guidance is vital for several stakeholders within the health system, each playing a crucial role in its effective execution.

Primary Users
- Hospital Administrators: Responsible for integrating the guidance into hospital operations.
- Emergency Response Teams: Directly interact with the planning document to execute drills and real-time responses.
- Health Department Officials: Oversee public health implications and regulatory compliance.
Scenarios of Usage
- Hospital administrators utilize the guidance to craft an overarching emergency response strategy.
- Health department officials reference the guidance to synchronize public health efforts with hospital actions during a pandemic.
Where applicable, utilize additional subsections to explore specific nuances, exceptions, or examples related to the guidance described.