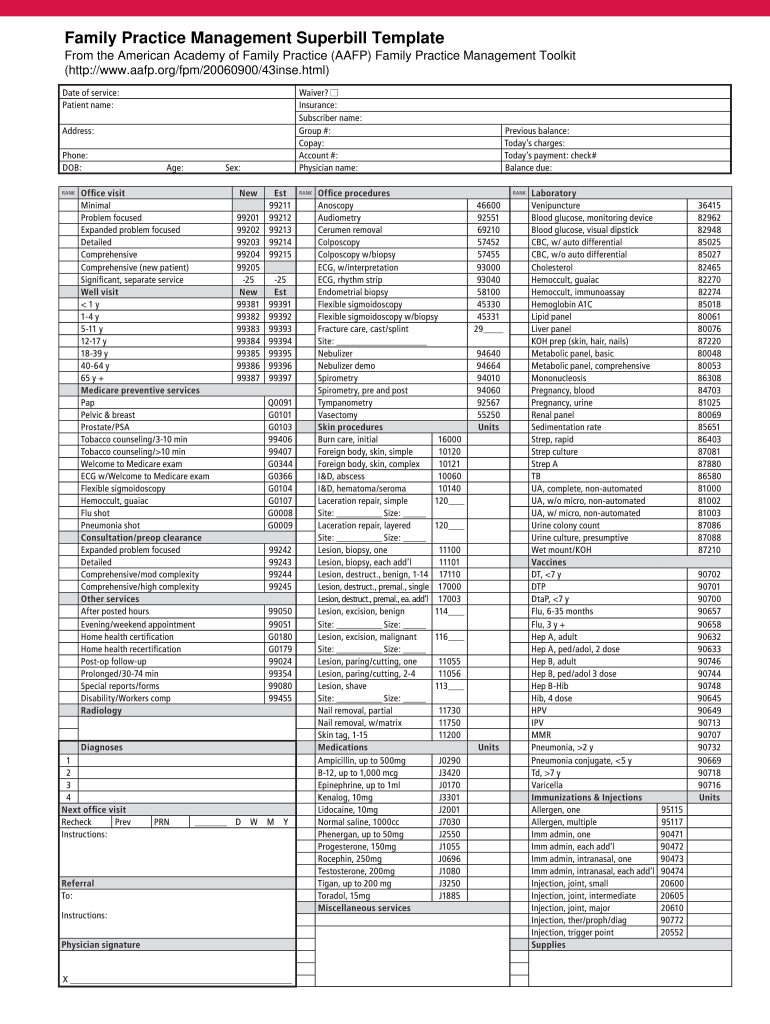
Definition and Meaning of a Superbill
A superbill is a detailed document used by healthcare providers to bill patients and insurance companies for services rendered. It serves as an essential tool in the medical billing process by itemizing the diagnosis, procedures performed, and associated costs. Though it is typically generated during a patient visit, it functions as a comprehensive record that combines both clinical and billing information.
Key Components of a Superbill
-
Patient Information: This section includes the patient's name, demographics, insurance details, and account number.
-
Visit Details: The date of service, place of service, and the names of healthcare providers involved are recorded here to accurately reflect the context of the visit.
-
CPT Codes and Description: Current Procedural Terminology (CPT) codes are crucial as they specify the services provided, from consultations to surgical procedures.
-
Diagnosis Codes: The International Classification of Diseases (ICD) codes explain the medical reasons for the patient’s visit and justify the services billed.
-
Modifiers: These codes provide additional detail about the services performed or indicate that a particular service was altered but not changed in its definition or code.
By including these comprehensive elements, the superbill can effectively streamline the claims submission process and provide detailed documentation for audits or insurance payment reviews.
Steps to Create a Medical Superbill
Creating a superbill involves several critical steps that ensure accuracy and compliance with billing regulations.
-
Gather Patient Information: Start by collecting essential patient demographic data, including name, address, date of birth, and insurance provider details.
-
Document Services Rendered: During the patient visit, take detailed notes on the services provided, including exams, treatments, and counseling.
-
Assign Appropriate Codes: Select the correct CPT and ICD codes that match the services and diagnoses recorded. This step is crucial to avoid billing errors and to enhance the likelihood of claim acceptance by insurance companies.
-
Review for Accuracy: Double-check the information for accuracy. Ensure that all services are captured and that codes are updated according to current standards.
-
Submit the Superbill: Once completed, the superbill can be submitted to the insurance company for reimbursement or given directly to the patient for out-of-pocket payments.
Importance of Superbills
Superbills play a pivotal role in the healthcare ecosystem for various reasons:
-
Facilitate Insurance Claims: They ensure that healthcare providers receive timely reimbursements and help patients understand their bills.
-
Medical Record Keeping: These documents serve as a vital part of the patient's medical record, providing essential information for future visits and treatments.
-
Compliance and Auditing: Superbills provide a reliable trail of services rendered, which is indispensable for audits, helping to maintain compliance with healthcare regulations.
-
Revenue Cycle Management: By utilizing superbills, healthcare facilities can improve their revenue cycle management, leading to more accurate financial forecasting and reduced billing problems.
Common Types of Superbills
Different healthcare specialties may use tailored superbills to better suit their billing needs. Here are some common types:
-
Primary Care Superbill: Typically includes a broad range of services that may be provided in a family practice setting.
-
Urgent Care Superbill: Designed specifically for urgent care facilities, this superbill focuses on acute medical conditions and associated treatment codes.
-
Lactation Superbill: Used by lactation consultants to outline services related to breastfeeding support and education.
-
Optometry Superbill: Tailored for eye care practitioners, including vision exams and eyewear prescriptions.
-
Psychotherapy Superbill: Designed for mental health professionals, emphasizing services related to therapy sessions and assessments.
Each variant is crafted to optimize billing according to the standards and codes relevant to the specific practice area.
How to Use a Superbill for Insurance Claims
Utilizing a superbill for insurance claims effectively involves understanding its components and how they align with insurance requirements.
Step-by-Step Instructions
-
Complete the Superbill: Fill in all necessary patient information, detailing the services and corresponding codes as outlined previously.
-
Distribution: Offer the completed superbill to the patient or submit it directly to the insurance provider, depending on the practice’s billing policies.
-
Check Claim Status: If submitting to an insurer, track the claim through the insurer’s claims portal or by contacting the insurance claims department.
-
Respond to Queries: Be prepared to answer any questions from the insurance provider regarding the superbill, including clarifying codes or services.
-
Reconcile Payments: After approval, reconcile payments received against the superbill to ensure that the documentation matches all transactions.
This structured approach not only simplifies the billing process but also minimizes errors and enhances the potential for timely reimbursements.
Legal Considerations Surrounding Superbills
Superbills must adhere to various legal and regulatory standards to ensure compliance with healthcare laws and regulations. This section highlights key legal aspects:
Important Legal Aspects
-
Compliance with HIPAA: Health Insurance Portability and Accountability Act (HIPAA) regulations mandate that patient data be kept confidential. Superbilling practices must protect this information.
-
Proper Coding: Incorrect coding can lead to legal ramifications, including audits or fines. Providers must remain updated on coding changes to maintain compliance.
-
Reimbursement Policies: Understanding insurance providers' reimbursement policies ensures that services billed through the superbill align with allowable charges, ultimately protecting against denials.
Awareness of these legal considerations ensures that healthcare providers can navigate the complexities of billing while safeguarding themselves and their patients from potential ramifications.