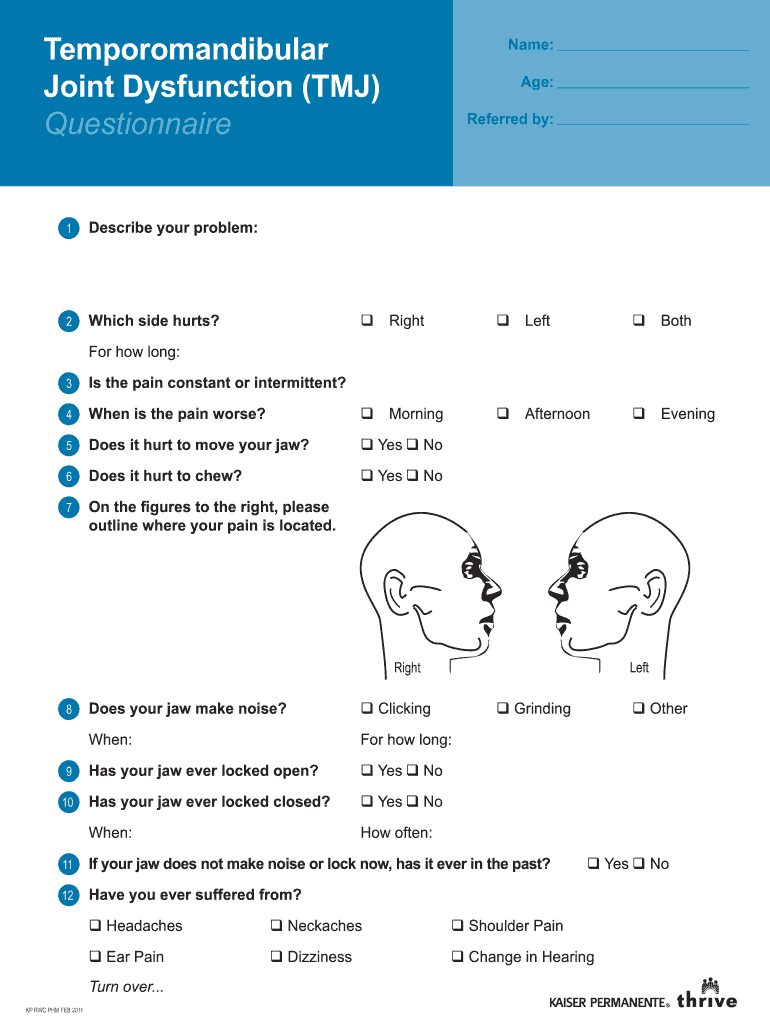
Overview of Temporomandibular Joint Questionnaire
The temporomandibular joint questionnaire is an assessment tool tailored for individuals experiencing symptoms related to temporomandibular joint dysfunction (TMJ). This questionnaire serves to gather crucial data on a patient's symptoms, allowing healthcare providers to form a comprehensive understanding of their TMJ-related issues.
Key Objectives of the Questionnaire
The primary aim of the temporomandibular joint questionnaire is to:
- Evaluate pain severity and location associated with the TMJ.
- Analyze the frequency and duration of symptoms over a specified period.
- Identify specific jaw movements that exacerbate discomfort or pain.
- Document any associated symptoms, such as headaches or ear pain.
- Assess previous treatments attempted and their effectiveness.
This thorough understanding enables practitioners to develop tailored treatment plans that address the unique needs of each patient.
Common Symptoms and Indicators
Patients often present a variety of symptoms that can be assessed through the questionnaire. Typical indicators include:
- Pain Location: Questions probe into whether pain is localized in the jaw, teeth, facial region, or neck.
- Symptom Frequency: Gathering information on how often symptoms occur can help in determining the severity and necessary interventions.
- Jaw Functionality: Evaluating the range of motion or any locking/clicking sensations in the jaw can assist in diagnosing TMJ issues.
- Associated Symptoms: Symptoms such as headaches, ear discomfort, and difficulty chewing are crucial in forming a complete clinical picture.
Undoubtedly, accurately capturing these details is vital for appropriate diagnosis and treatment recommendations.
Types of Assessments Included
The temporomandibular joint questionnaire may include several specific assessments to better understand the patient's condition. Here are a few common components:
- Pain Scales: Patients may be asked to rate their pain on a scale of one to ten, providing quantifiable data on discomfort.
- Jaw Mobility: Questions that test the ability to open and close the jaw or move side to side are central to the evaluation.
- Functional Limitations: Surveys inquire about activities that trigger or exacerbate symptoms, including eating, speaking, or yawning.
- Treatment History: Previous treatments—such as physical therapy, medications, or dental procedures—are documented to identify what might have been beneficial or not.
These components are essential to gauge the overall impact of TMJ dysfunction on daily living.
Relevance of Patient History
Understanding a patient’s history is a critical aspect of the temporomandibular joint questionnaire. Important elements to consider include:
- Prior Diagnoses: Any past medical or dental conditions that relate to jaw issues can inform treatment.
- Previous Treatments: Information on treatments previously attempted and their outcomes guide future therapeutic decisions.
- Family History: A familial tendency towards jaw disorders can influence diagnosis and treatment pathways.
- Lifestyle Factors: Habits such as grinding teeth (bruxism) or a history of trauma to the jaw can significantly influence TMJ health.
A well-rounded patient history allows healthcare providers to formulate precise and effective treatment strategies.
Evaluation and Next Steps
Once the temporomandibular joint questionnaire is completed:
- Initial Review: A healthcare provider assesses the responses for common indicators of TMJ dysfunction.
- Diagnosis: The accumulated data provides a basis for a possible diagnosis, helping to understand whether TMJ dysfunction is likely.
- Further Testing: Depending on the findings, additional evaluations may be needed, including physical examinations or imaging studies such as X-rays.
- Tailored Treatment Plans: Treatment might include lifestyle adjustments, physical therapy, medication, or in some cases, surgical options, determined by the severity of the condition.
By systematically evaluating the data collected through the questionnaire, clinicians are better equipped to recommend personalized care plans suited to each patient’s specific needs.
Resources for Follow-up and Management
Post-evaluation considerations for ongoing management may include:
- TMJ Exercises: Resources like a "TMJ exercises PDF" provide patients with physical techniques to enhance jaw mobility and reduce pain.
- Physical Therapy Evaluation Templates: Utilizing tools like the TMJ physical therapy evaluation template supports healthcare providers in cataloging patient progress.
- Assessment Documentation: Keeping thorough TMJ assessment documentation aids in tracking symptom evolution and treatment effectiveness over time.
These resources are instrumental in empowering patients toward active participation in their treatment, potentially leading to better outcomes.