



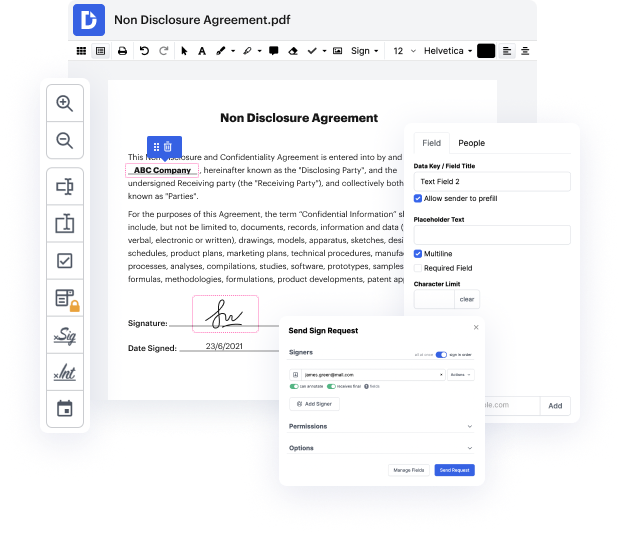
DocHub enables you to change photo in Medical Invoice quickly and quickly. No matter if your form is PDF or any other format, you can effortlessly alter it using DocHub's easy-to-use interface and robust editing features. With online editing, you can change your Medical Invoice without downloading or setting up any software.
DocHub's drag and drop editor makes personalizing your Medical Invoice straightforward and efficient. We securely store all your edited documents in the cloud, enabling you to access them from anywhere, anytime. Moreover, it's effortless to share your documents with parties who need to check them or add an eSignature. And our native integrations with Google services help you transfer, export and alter and endorse documents right from Google applications, all within a single, user-friendly platform. Additionally, you can quickly turn your edited Medical Invoice into a template for future use.
All executed documents are securely stored in your DocHub account, are effortlessly managed and shifted to other folders.
DocHub simplifies the process of completing form workflows from day one!
Matt from EAT Tactics introduces a tutorial on understanding claim rejection reasons, highlighting the clearinghouse’s 20 years of experience and connections with numerous payers. He notes that varying claim submission rules across payers are often the reason for viewing the video. Matt emphasizes the importance of subscriber engagement, encouraging viewers to subscribe and hit the alert bell for new content. The tutorial will provide insights into common claim requirements and rejection reasons encountered at the clearinghouse level, drawn from extensive experience in submitting claims on behalf of healthcare providers.
At DocHub, your data security is our priority. We follow HIPAA, SOC2, GDPR, and other standards, so you can work on your documents with confidence.
Learn more



